 
But please believe me when I say Diastasis Recti surgery is about SO much more than appearances. HGTV has brainwashed me into thinking that before and after shots are everything, so I’ll start with the good stuff. 
Diastasis Surgery Photos – Before and After ( MORE Before/ After Photos at the END OF THIS POST) My surgeon repaired both a hernia and my diastasis recti gap. In most cases, it is secured to the underlying fascia at the three, six, and nine o'clock positions.In January of 2020, I had Diastasis Recti Surgery. Excess abdominal skin was excised in the normal fashion and the umbilicus delivered through a midline incision. Plication of the rectus fascia was then performed using the previous markings, which allowed for symmetrical placation of the anterior sheath. The midline laparotomy fascial incision was then closed with running monofilament suture. The hernia was then repaired with interrupted, nonabsorbable monofilament sutures ( Figure 1, A-D). The fascial defect was identified and the hernia reduced from the undersurface of the umbilicus either in the pre- or intraperitoneal space. A 3- to 4-cm midline longitudinal laparotomy incision was then made through the linea alba, beginning 2 cm inferior to the umbilical stalk. The fascial plication was marked based on the degree of anterior fascial laxity. The abdominal flap was raised at the level of the anterior sheath to the xyphoid centrally and the costal margins laterally. The abdominal flap was elevated and the umbilicus was dissected from the anterior abdominal wall flap while leaving intact the fascial attachments of the umbilical stalk at its base. We present a simplified surgical technique that avoids any fascial incisions immediately adjacent to the umbilicus, thereby maintaining maximal blood supply to the umbilical stalk and minimizing the risk of umbilical necrosis. 3–8 This increased risk has lead many surgeons to either avoid repair of these hernias or perform a two-stage procedure for correction. Therefore, abdominoplasty and umbilical hernia repair, when performed simultaneously using the traditional aforementioned techniques, can potentially compromise the vascular supply to the umbilicus, resulting in tissue necrosis. Because of this extensive dissection, the blood supply to the umbilicus is primarily derived from the surrounding attached skin via the subdermal plexus. Standard repair of umbilical hernias involves fascial incisions immediately adjacent to the abdominal wall defect and extensive dissection in preparation for repair. As a result, the umbilicus maintains its only blood supply from the underlying fascial attachments via the umbilical stalk. 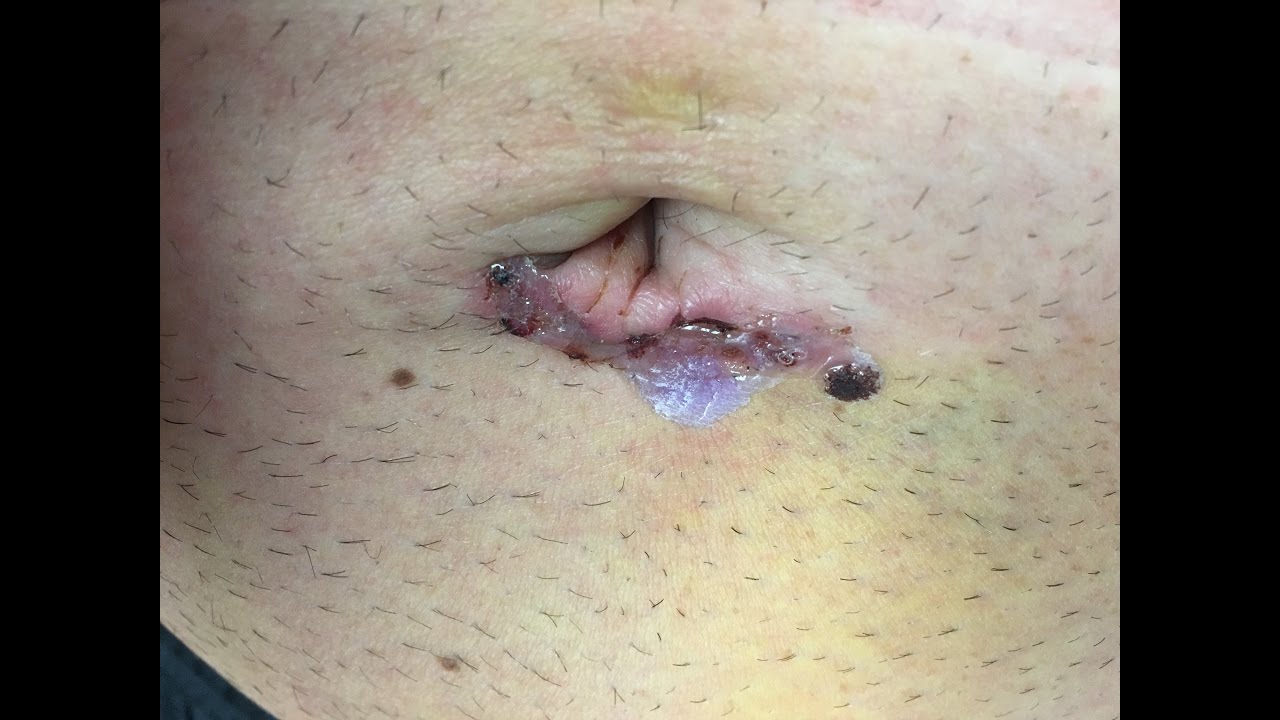
Traditional surgical techniques for performing an abdominoplasty include skin incisions circumferentially around the umbilicus, resulting in complete detachment of the umbilicus from the anterior abdominal flap. 
However, undertaking such a repair is not without potential consequences. The identification of an umbilical or periumbilical hernia while performing an abdominoplasty provides the plastic surgeon an opportunity to surgically correct the fascial defect, which in many cases significantly contributes to the overall appearance of the anterior abdomen. One of the most common locations for a hernia to occur is in the umbilical and periumbilical area. In fact, hernias are often diagnosed on clinical examination or are encountered intraoperatively during an abdominoplasty. 1–5 A frequently-encountered problem associated with the occurrence of fascial laxity or diastasis is abdominal wall hernias. One of the primary indications for the procedure is skin and fascial laxity, which is often found in multiparous women. Abdominoplasty is one of the most common aesthetic procedures performed in the United States. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
